
As artificial intelligence (AI) expands into all aspects of patient care, it is more important than ever that clinicians understand how these algorithms work and what they can and cannot do, according to Tyler Berzin, MD, associate professor at Harvard Medical School and director of the advanced endoscopy fellowship at Beth Israel Deaconess Medical Center.
Dr. Berzin spoke with DDW News about current and future impacts of AI in gastroenterology and what clinicians need to be aware of when using AI in their practice.
DDW: How is artificial intelligence currently used in gastroenterology?
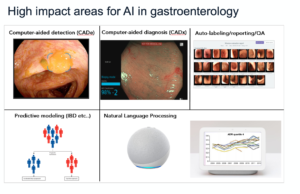
Berzin: Colon polyp detection is very much the ‘tip of the spear’ for AI in gastroenterology. Computer-aided detection (CADe) for polyps will likely be the first encounter that most practicing gastroenterologists have with AI in clinical practice. This is just the first AI tool of many that will eventually be introduced to the endoscopy suite.
DDW: What are some of the biggest impacts AI is making in gastroenterology?
Berzin: The potential impacts are innumerable. Computer vision for detection and diagnosis in GI endoscopy is generating the most excitement.
Personally, I am even more interested in tools that can help physicians disconnect from the keyboard and screen and re-focus on our patients. Most of us didn’t go to medical school expecting to spend so much of our day on data entry, transcribing our analog reality into a digital record. We should invest in tools that reduce the documentation burden for physicians; for example, tools that could complete an endoscopy report in a semi-automated fashion or ambient clinical intelligence that can listen to the clinical visit and create a clean and organized visit note without the need for dictation.
DDW: Your talk focuses on how AI works. Why is it important that clinicians understand how AI algorithms work?
Berzin: In medical school, we learn statistics to help inform our clinical decision-making and to support our ability to evaluate new clinical evidence. I think it will be equally important that physicians develop a basic understanding of AI and machine learning so that we can interact with these tools in clinical practice.
Berzin: Human intelligence is robust, and AI is quite fragile. Subtle changes in how an X-ray image is processed or how the light spectrum is displayed during endoscopy won’t typically throw off a physician, but seemingly small perturbations like these can potentially spell ruin for an AI algorithm.
AI tools can harness incredible computational power to recognize patterns or make certain clinical predictions, but these powerful tools utterly lack common sense. There must be a synergy between physicians and AI. Artificial intelligence is really just another tool to be wielded thoughtfully and ethically in the service of our patients.
DDW: Given these limitations, how can clinicians ensure that their AI programs are robust and working correctly?
Berzin: Careful monitoring is necessary and required by regulatory agencies to ensure that medical AI algorithms continue to perform as expected over time. For instance, if we’re about to upgrade our fleet of colonoscopes to a newer model from a different manufacturer, we need to ensure that our AI polyp detection works equally well with the new equipment.
DDW: How do you see artificial intelligence evolving in the future?
Berzin: I think there is enormous potential for AI to play a critical role in all phases of clinical care — from detection and diagnosis in the endoscopy suite to predictive modeling and treatment planning for IBD and liver disease.
Additionally, natural language processing may allow us to more easily manage our own practice data so that we can measure, report and compare our own quality metrics more easily than is currently possible.
Dr. Berzin’s oral presentation, “The nuts and bolts of artificial intelligence: How does it all work?” takes place on Sunday, May 22, at 2 p.m. PDT as part of the clinical symposium, “Innovation in Artificial Intelligence: Implications for Clinical Practice.”



