
Patients with pancreatic cancer were six times more likely to have had gallstone disease in the year prior to diagnosis, compared to non-cancer patients, according to new data being presented at Digestive Disease Week® (DDW) 2022.
“Anecdotally, the connection between gallstone disease and pancreatic cancer comes up a lot,” said Marianna Papageorge, MD, research fellow at Boston Medical Center and lead researcher of the study. “But it has never been compared to a non-cancer population, and the timing of the association wasn’t clear.”
The study compared the incidence of gallstone disease, which included gallstones and inflammation of the gallbladder, and gallbladder removal (cholecystectomy), between patients with pancreatic cancer (n = 18,700) and a non-cancer cohort consisting of an average of 99,287 patients per year from the SEER-Medicare database (2008-2015).
Those with pancreatic cancer were almost six times more likely than the general population to have been hospitalized for gallstone disease in the year prior to their cancer diagnosis. Specifically, in the year prior to diagnosis:
- The incidence of gallstone disease in patients with pancreatic cancer was 4.7 percent, compared to 0.8 percent per year in the non-cancer cohort.
- The incidence of cholecystectomy in patients with pancreatic cancer was 1.6 percent, compared to 0.3 percent per year in the non-cancer cohort.
Among those with pancreatic cancer:
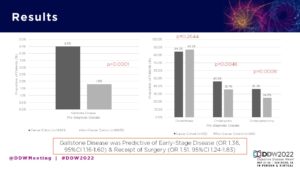
- Patients with prior gallstone disease were more likely to be diagnosed with Stage I-II disease compared to those without gallstone disease (47.9 percent vs. 40.5 percent, p<0.0001).
- Patients with prior gallstone disease were more likely to have undergone pancreaticoduodenectomy compared to those without gallstone disease (17.6 percent vs. 12.9 percent, p<0.0001).
Dr. Papageorge hopes that these data will improve differential diagnosis of pancreatic cancer, potentially providing an opportunity for earlier diagnosis and intervention.
“Pancreatic cancer often presents with insidious symptoms. A better understanding of the predictors can help to broaden a differential diagnosis,” Dr. Papageorge said. “If patients have other risk factors for pancreatic cancer, the presence of gallstone disease may make their physician think twice about screening.”
However, gallstone disease is just one piece of the puzzle. Dr. Papageorge stressed that the presence of gallstone disease should not in and of itself raise any red flags about the potential for pancreatic cancer, but does support the need for comprehensive follow-ups.
“Gallstones do not lead to pancreatic cancer,” Dr. Papageorge said. “Pancreatic cancer is very rare, and many people have gallstone disease. This type of data should motivate us to ensure that patients have good follow-up care, that they’re seeing a primary care physician more regularly and following up with their surgeon if they had their gallbladder removed. That continuation of care will help lead to earlier diagnosis.”
Dr. Papageorge will present data from the study, “Gallstone disease in the year prior to pancreatic cancer diagnosis: an opportunity for action,” abstract 761, on Monday, May 23, at 4:12 p.m. PDT.




One Response
Do you have data about ethnicity? The biliary disease is a preponderant latin american disease .