The growing availability of safe and effective medications for people with hepatitis C virus (HCV) underscores the importance of clinicians understanding whom to treat and specifically how to do so, according to Brian L. Pearlman, MD, FACP, FAASLD, AAHIVS, medical director at the Center for Hepatitis C at Wellstar Atlanta Medical Center and professor of medicine at Medical College of Georgia and Emory School of Medicine.
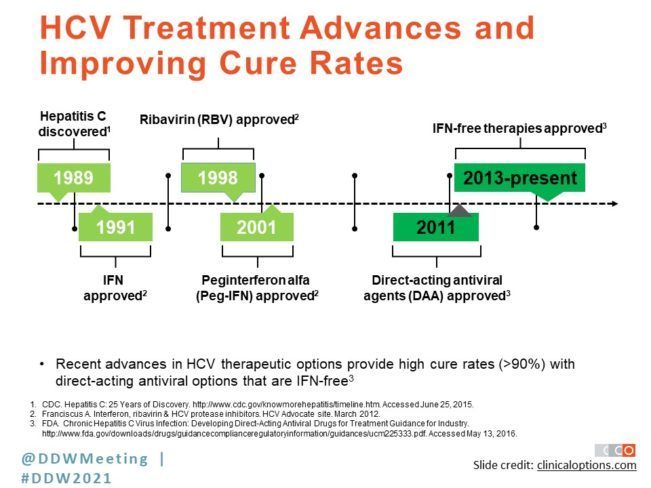
“Understanding the history is important, because it shows how far we’ve come,” said Dr. Pearlman, who presented on HCV treatment at DDW® 2021. “To go from a disease that we did not even understand in the mid-1970s to early 1980s, to now having developed well-tolerated therapies that are over 95% effective is remarkable; very few advances in medicine have come so quickly. And HCV is now the only curable chronic illness of which I’m aware.”
Dr. Pearlman identified five HCV populations of whom clinicians should take particular notice:
- Treatment-naïve patients. Numerous phase 3 clinical trials support the effectiveness and tolerability of antiviral drugs in treatment-naïve patients of every genotype and in compensated cirrhosis and non-cirrhosis.
- Treatment-experienced patients. FDA-approved medications, such as combination sofosbuvir-velpatasvir-voxilaprevir, are now available for patients who have failed other established treatments. Recent research also shows that certain viral mutations (called resistance-associated substitutions) in people who have failed prior therapies are not a barrier to these patients benefitting from medication.
- People with decompensated cirrhosis. These patients should be treated by an experienced provider and, ideally, in a liver transplant center. Antiviral regimens are available and could help improve Child-Pugh score, and protease inhibitors should not be used in this population.
- People with renal disease. This was previously considered a difficult-to-treat population, said Dr. Pearlman, but direct-acting antivirals can now be used — and do not need to be adjusted — in people with a glomerular filtration rate under 30 ml/min.
- People who inject drugs (PWIDs). Although the treatment and cure rate for HCV is good, about half of all people with HCV in the U.S. don’t know they have the disease, said Dr. Pearlman. And underdetection is particularly common among marginalized populations, like PWIDs. But ensuring these individuals receive timely treatment is imperative to reducing the overall prevalence of HCV in this country.
Dr. Pearlman’s oral presentation of “Evolution of hepatitis C: Drugs, patients and guidelines” took place Sunday, May 23, at 5:30 p.m. EDT, as part of the AASLD session “Chronic HCV Infection in 2020: What Does the Future Hold?”



