Wading through the multiple professional guidelines for managing pancreatic cysts can be confusing and intimidating for gastroenterologists, according to Vanessa Shami, MD, professor of medicine at the University of Virginia Medical Center. At Digestive Disease Week® (DDW) 2023, Dr. Shami presents the similarities and differences among the guidelines to help clinicians identify precancerous cysts and create a plan to manage them.
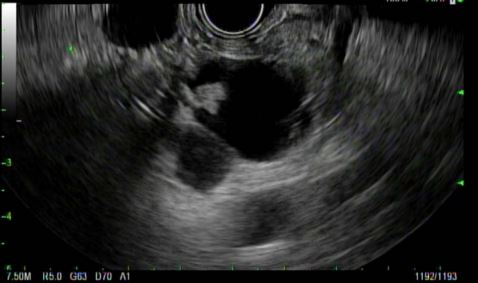
“Pancreatic cysts are extremely common and can pose a major dilemma for gastroenterologists,” said Dr. Shami. “Although the majority will not result in cancer, patients understandably get anxious about anything related to a pancreatic lesion. As gastroenterologists, it is important to decide whether a cyst is premalignant and devise a proper surveillance plan.”
Dr. Shami discusses pancreatic cyst guidelines published by the following groups.
- The American College of Gastroenterology (published in 2018)
- The American Gastroenterological Association (published in 2015)
- The European Study Group on Cystic Tumours of the Pancreas (last published in 2018)
- International Consensus Guidelines (also known as the Sendai guidelines; last published in 2017)
With all these guidelines, how can clinicians determine the best course of action for their patients?
“There are so many guidelines to choose from, and they all approach pancreatic cysts differently,” Dr. Shami explained. “My goal is to simplify the guidelines for clinicians because, at a high level, they all have a common theme.”
Dr. Shami notes that, at their core, the guidelines are all trying to help physicians answer two fundamental questions: Is a cyst at high risk of malignancy? And how should gastroenterologists develop a management plan?
Risk of Malignancy
The guidelines are fairly consistent in defining the high-risk features of pancreatic cysts that would warrant treatment. When high-risk features are detected, surgery or endoscopic ultrasound (EUS) may be recommended. If no high-risk features are found, a surveillance plan may be put in place to prevent the development of pancreatic cancer.
Some high-risk stigmata include:
- Obstructive jaundice
- Cyst size (≥3 cm in most guidelines)
- Presence of a mural nodule or solid component
- Dilation of the main pancreatic duct
- Positive cytology on cyst fluid aspiration
If surveillance or treatment is required, what should a management plan look like?
The guidelines vary in devising a surveillance and management plan for high-risk cysts. They differ in the specifics of:
- How often to follow patients
- When to consider EUS
- When to consider resection
In addition to the biological risk factors noted above, clinicians must also weigh other patient-specific factors to tailor their plans to the patient’s risk tolerance and preferences. These factors include:
- Morbidity and mortality of pancreatic surgery
- The psychological burden of routine surveillance
- Patient willingness and/or candidacy for pancreatic surgery or chemotherapy
Ultimately, Dr. Shami advises that clinicians base their management plans on guidelines and be able to provide a rationale for their decisions. “If you miss cancer, it’s a big liability,” Dr. Shami said. “It’s extremely important to follow a guideline and document the rationale for your management plan.”
Dr. Shami has consulted for Cook Medical, Olympus and Boston Scientific.
Dr. Shami’s oral presentation, “Navigating guidelines on pancreatic cysts” on Tuesday, May 9, at 4:02 p.m. CDT, is part of the session “ASGE & Society of Gastrointestinal Endoscopy of India (SGEI) International Symposium: Advances in Pancreato-Biliary.”
If you’re attending DDW, your registration includes access to a recording of this session, available to watch at your convenience until May 17, 2024. Session captures will be released 24 hours after the session ends. Non-attendees can also purchase access to DDW On Demand to watch session recordings after DDW ends.