
The American Association for the Study of Liver Diseases (AASLD) recently approved new guidance on the diagnosis and management of primary sclerosing cholangitis (PSC) and cholangiocarcinoma.
DDW News spoke with David N. Assis, MD, associate professor of medicine at the Yale School of Medicine, who presented an overview of the new guidance during Digestive Disease Week® (DDW) 2022.
DDW: What was the impetus for updating the guidance at this time?
Assis: Managing patients with PSC remains very challenging. The new guidance provides a data-driven update on PSC and includes the first focused guidance from the AASLD dedicated to the diagnosis and management of cholangiocarcinoma, a frequent complication of PSC.
We hope that the new guidance will be an informative and useful tool for clinicians, patients and researchers to provide high-quality care for patients with PSC.
DDW: How does the new guidance differ from the 2010 guidance on PSC?
Assis: There are several updates regarding the diagnosis of PSC, including an emphasis on high-quality magnetic resonance imaging (MRI) as the seminal diagnostic tool and that endoscopic retrograde cholangiopancreatography (ERCP) should no longer be performed as part of the diagnostic process.
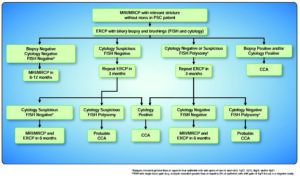
The guidance also introduces a new term, “relevant stricture”, defined as any biliary stricture of the common hepatic duct or hepatic ducts associated with signs or symptoms of obstructive cholestasis and/or bacterial cholangitis. This marks a shift from the older term, “dominant stricture,” which described the caliber of bile ducts measured during ERCP. Evaluating patients with relevant strictures is critical because this is often a presentation of early cholangiocarcinoma.
The guidance also strongly emphasizes that all patients with PSC should be considered for clinical trials given the lack of proven effective medical therapy. For patients who are ineligible for clinical trials, ursodeoxycholic acid (UDCA) in moderate doses can be considered. This is in contrast to the previous guidance, which recommends against UDCA, based on data showing the harms of high-dose UDCA.
The new guidance additionally discusses emerging clinical risk tools for prognostication in PSC. Lastly, the guidance highlights recent updates to the policy of the United Network for Organ Sharing (UNOS) for liver transplantation in the context of PSC.
 DDW: What does the new guidance add with regard to cholangiocarcinoma?
DDW: What does the new guidance add with regard to cholangiocarcinoma?
Assis: Correct and early diagnosis of cholangiocarcinoma is critical to allow for the best treatment options, including liver resection and liver transplantation. To this end, the new guidance specifically recommends that florescent in situ hybridization (FISH) be performed, along with standard brush cytology, when evaluating relevant strictures using ERCP. The guidance also contains an excellent discussion with clear, practical statements devoted to the management of cholangiocarcinoma in a manner that will be quite useful for hepatologists and all providers who participate in the complex, multi-disciplinary care required for these patients.
DDW: How do you expect the new guidance will impact patient care and management?
Assis: The new guidance highlights current best practices for the diagnosis and management of patients with PSC, a challenging disease that requires longitudinal care and teamwork among clinicians, patients and caregivers.
We anticipate that the novel specific guidance devoted to cholangiocarcinoma in its own right will bring much-needed attention to this very challenging cancer and improve patient outcomes by communicating the most current diagnosis and management methods.
Dr. Assis will give the oral presentation, “Primary sclerosing cholangitis cholangiocarcinoma,” on Monday, May 23, at 4:45 p.m. PDT as part of the AASLD Practice Guidelines Workshop.



