
Active observation and repeat evaluation may be a useful strategy to diagnose acute appendicitis in patients with inconclusive ultrasound findings, according to a new study presented at Digestive Disease Week® (DDW) 2022.
“Diagnosing acute appendicitis typically involves conducting a computed tomography (CT) scan on every patient if clinical, laboratory and ultrasound evaluation are inconclusive,” said Raminta Luksaite-Lukste, lead researcher on the study and PhD student at Vilnius University in Lithuania. “This strategy of conditional CT scans keeps our negative appendectomy rate low, but we also end up conducting CT scans on many more patients than we need to — in more than 50 percent of patients, CT scans do not detect any acute pathology.”
Researchers conducted a prospective randomized trial at Vilnius University Hospital to compare the impact of active surveillance and conditional CT scans on CT rates, negative appendectomy and complicated acute appendicitis cases. They also evaluated the role of repeated laboratory tests and ultrasound in diagnosing acute appendicitis.
The study included 160 patients who presented to the emergency department with symptoms consistent with acute appendicitis. Patients were only included if they were deemed to be at low-to-medium risk of having acute appendicitis, defined as those experiencing symptoms for less than 48 hours without markers of high inflammation. After a transabdominal ultrasound (TUS), those with inconclusive findings were randomized to two groups:
- Control group: All patients underwent a CT scan, per the hospital’s standard diagnostic protocol.
- Active surveillance group: Patients were observed for 8 to 12 hours and then re-evaluated via laboratory testing and TUS.
- CT scan rate was lower in the observation group (35 percent) than in the control group (100 percent).
- There was no difference in negative appendectomy rate between the observation group (1.2 percent) and the control group (0).
- There was no increase in the rate of complicated acute appendicitis cases between the observation group (6.3 percent) and the control group (13.8 percent).
- Change in C-reactive protein prior to and after the observation period was able to distinguish between patients with and without acute appendicitis.
These results indicate that active observation may be an effective strategy in patients suspected of acute appendicitis.
“Our study shows that CT scans are not always necessary to diagnose acute appendicitis,” said Luksaite-Lukste. “Our active observation protocol has a number of benefits to both hospitals and patients. First, it provides an effective alternative for hospitals that do not have access to CT 24/7, and conducting fewer CT scans can decrease hospital costs. In addition, choosing observation over a CT scan can spare young patients from the effects of ionizing radiation and unnecessary surgery-related complications.”
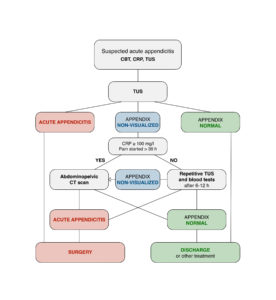
Luksaite-Lukste proposed an alternative algorithm for diagnosing acute appendicitis (image) based on their findings.
Luksaite-Lukste will present the e-poster “The value of observation strategy in diagnostics of acute appendicitis: prospective randomized clinical trial” on Saturday, May 21, at 12:30 p.m. PDT.




One Response
Did you consider some scale of appendicits?