
New research to be presented at Digestive Disease Week® 2021 suggests the glucagon-like peptide-1 receptor agonist (GLP-1) semaglutide is a safe and effective adjunct to endoscopic sleeve gastroplasty (ESG). In fact, the analog could help patients undergoing ESG achieve weight loss comparable to that seen with the highly successful but far more invasive laparoscopic sleeve gastrectomy (LSG).
“I found that by adding the GLP-1 analog, we could take it to the next step,” said Anna Carolina Hoff, MD, lead researcher on the study and founder and clinical director of Angioskope Brazil. “We went from the procedure producing 16 percent to 18 percent of weight loss [without semaglutide] to almost 27 percent of total body weight loss, which is excellent.”
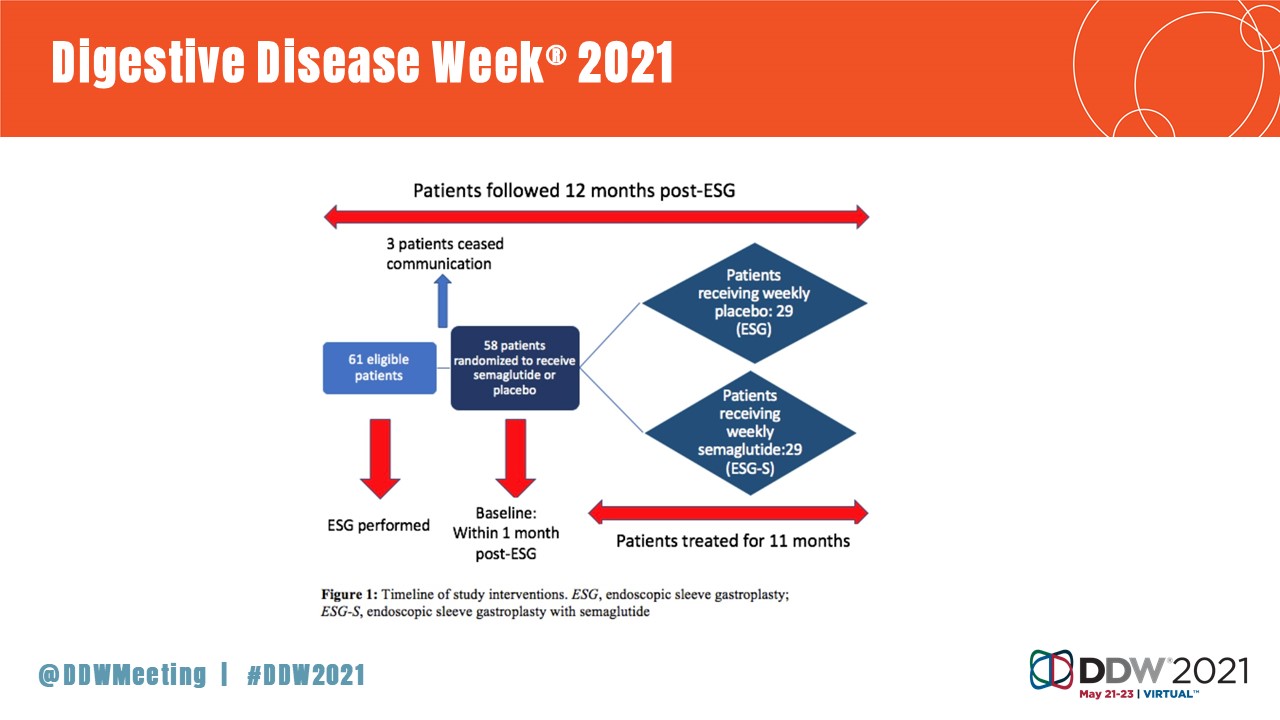
Fifty-eight patients undergoing ESG were randomly given either weekly semaglutide injections or placebo starting one-month following their procedure. Patients in both groups underwent the same suturing patterns, had the same diet and exercise prescriptions and were followed by the same treatment team. Results at 12 months showed:
- Total body weight loss with ESG plus semaglutide was 26.7 percent, in comparison to 19.6 percent in the placebo group. Total body weight loss seen with LSG is usually around 20 percent.
- The percent of excess weight loss was 86 percent in the treatment group and 60 percent in the placebo group.
- Semaglutide was well-tolerated with no serious adverse effects. And because semaglutide is a weekly, rather than daily injection, the patient burden was low.
“GLP-1 analogs are a safe class of drugs for either diabetic patients or nondiabetic patients,” added Dr. Hoff, noting that semaglutide did not lead to hypoglycemia. “But above all, they are analogs to a natural hormone, so they work properly without causing harm to the patient.”
“People cannot think we have found a cure for obesity and that combined therapies are a magic wand,” said Dr. Hoff. “Right now, we have great results, and we are trying other hormones to combine with GLP-1 analogs. I think it’s just the beginning. But other centers have to replicate our results too to conclude we are on the right path.”
Dr. Hoff’s oral presentation of “Semaglutide in association to endoscopic sleeve gastroplasty: Taking endoscopic bariatric procedures outcomes to the next level” will take place on Sunday, May 23, at 12:15 p.m. EDT, as part of the ASGE Bariatric Poster Session.



