
Gastroenterologists and hepatologists have a unique opportunity to significantly improve the quality of life in patients with cirrhosis, according to Elliot Tapper, MD, associate professor at the University of Michigan, who speaks on the topic during Digestive Disease Week® (DDW) 2023.
“This is an unprecedented time in the management of cirrhosis,” said Dr. Tapper. “The demand for our services is increasing as the prevalence of cirrhosis rises, and our ability to meaningfully help our patients has never been stronger.”
Dr. Tapper outlines 10 considerations for gastroenterologists and hepatologists managing patients with cirrhosis.
- Nutrition. Dr. Tapper advises counseling patients to eat a high-protein diet and providing resources on good sources of protein. “Everyone with cirrhosis needs to eat a high-protein diet and a late-night snack,” he said.
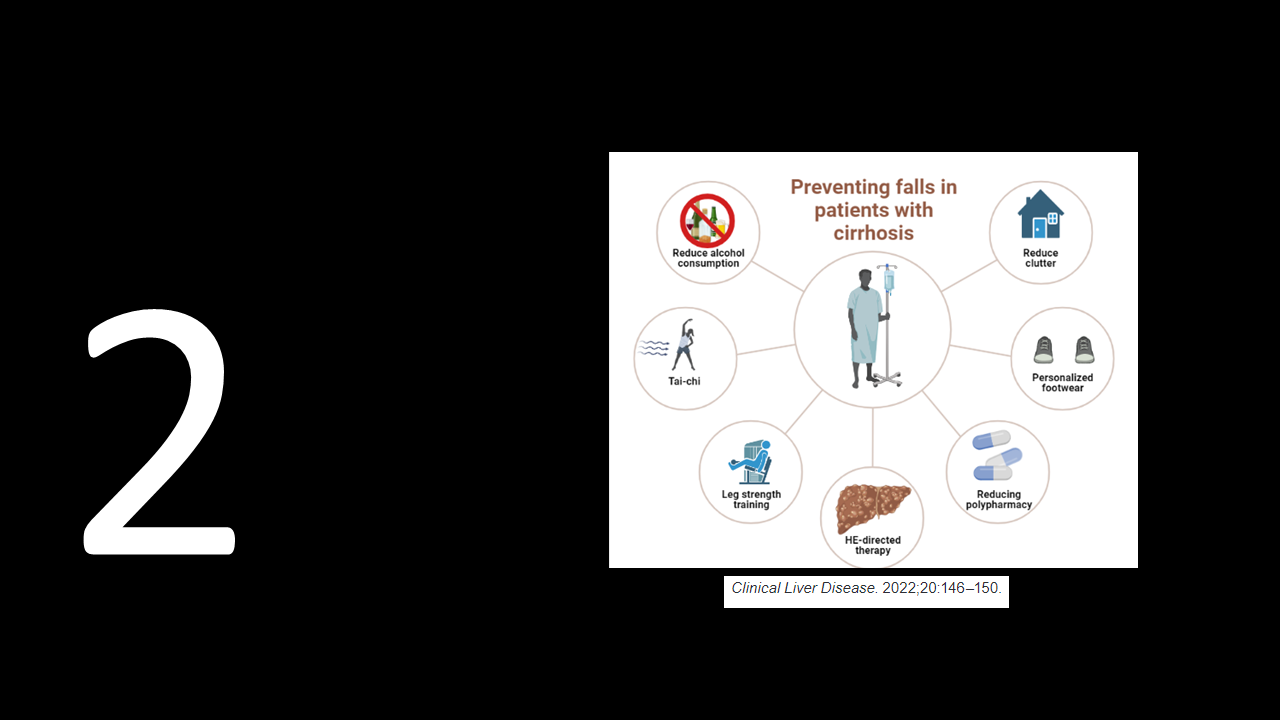
- Exercise. Patients with cirrhosis can experience muscle loss and weakness and are also at risk of fall-related injuries. He recommends providing resources, such as videos for patients to do home-based exercises (cirrhosiscare.ca for example), and talking about ways to prevent falls (Tai chi included).
- Pre-op stratification with VOCAL-Penn. The VOCAL-Penn score is an online calculator that predicts post-operative mortality in patients with cirrhosis that incorporates the type of surgery as well as patient- and disease-related factors. The predictions can be used to risk-stratify patients and help inform whether surgical or nonsurgical options should be considered.
- Phosphatidylethanol (PEth) testing to detect alcohol use, monitor patients (with their awareness) and classify the cause of liver disease.
- Effective pharmacotherapy for alcohol use disorders. Therapies such as naltrexone have shown to be highly effective in helping patients maintain abstinence, according to Dr. Tapper. He presents recent data from a retrospective cohort study that showed that medications for alcohol use disorder were also associated with improved survival in patients with alcohol-associated cirrhosis.
- Preventing decompensation. Tapper presents data from cohort studies and randomized trials showing that β blockers can prevent decompensation in those with compensated cirrhosis.
- Education. Educating not only patients but also their caregivers is critical. Dr. Tapper recommends that physicians have a set of resources ready and available to distribute and make sure to streamline their discussions.
- Addressing under-recognized symptoms. Patients with cirrhosis suffer from a host of symptoms related to their liver disease, including sleep dysfunction, sexual dysfunction, muscle cramps, itching and pain. Addressing these symptoms can go a long way in improving quality of life.
- De-prescribing medications. Dr. Tapper advises providers to avoid the use of common agents that can cause damage in patients with cirrhosis. For example, nonsteroidal anti-inflammatory drugs can increase the risk of acute renal failure and proton pump inhibitors are associated with an increased risk of infection and decompensation.
- Make lactulose more palatable. Lactulose has been shown to improve sleep quality and quality of life in patients with cirrhosis, according to Dr. Tapper. He describes ways to make it more palatable for patients.
Dr. Tapper notes that these measures represent an expansion of the role of gastroenterologists in managing compensated cirrhosis beyond the procedure-heavy focus of ultrasounds and cancer screenings.
“We need to intensify care and the amount of information provided to patients, even when they present in a compensated state,” he said. “Patients with cirrhosis are scary to their other doctors. Most elements of cirrhosis care cannot be feasibly deferred to others. It is incumbent on us as gastroenterologists to expand what we traditionally view as our responsibility. We can streamline these interventions so that they take a limited amount of time but have a massive impact on our patients’ quality and quantity of life.”
Dr. Tapper’s oral presentation, “Approach to your cirrhosis patient – top 10 dos and don’ts” on Monday, May 8, at 8:05 a.m. CDT is part of the session “AASLD Hepatology for Gastroenterologists Symposium.”
If you’re attending DDW, your registration includes access to a recording of this session, available to watch at your convenience until May 17, 2024. Session captures will be released 24 hours after the session ends. Non-attendees can also purchase access to DDW On Demand to watch session recordings after DDW ends.



